The Sendai Framework for Disaster Risk Reduction ("the Sendai Framework"), a set of guidelines for international disaster risk reduction ("DRR") initiatives, calls for multi-hazard approaches to pandemics, infectious diseases and other biological disasters as well as to natural disasters, i.e., for systematic management of a wide range of disasters. This constitutes a useful approach for reinforcing measures to combat COVID-19 and other infectious diseases, as it enables responses to spillover, cascading, compound and complex damage, and application of a significant track record of natural disaster management to battling infectious diseases. Stepping up approaches to multiple hazards inclusive of pandemics will require international cooperation in analyzing measures, drawing out the lessons to be learned, and supporting capacity-building in other countries.1
1. The multi-hazard approach called for by the Sendai Framework
The Sendai Framework presents guidelines for national and local government initiatives. Adopted by UN member states at the Third World Conference on Disaster Risk Reduction held in Sendai in 2015, the Sendai Framework presents seven targets, aiming 1)-4) to reduce disaster damage, 5) to create DRR plans and strategies, 6) to enhance international cooperation, and 7) to increase the availability of early warning systems and disaster risk information. The Framework posits 1) understanding disaster risk, 2) strengthening disaster risk governance, 3) investing in DDR and 4) enhancing disaster preparedness and "building back better" (Figure 1) as priorities for action to achieve these targets. Ultimately, however, these are merely guidelines and roadmaps that lack the coercive power of an international pledge.
The Sendai Framework covers natural disasters and man-made accidents (e.g., industrial accidents) as well as related environmental, technological and biological disasters (e.g., infectious diseases and pandemics). The inclusion of biological disasters can be attributed to lobbying by countries that experienced Ebola hemorrhagic fever, MERS (Middle East respiratory syndrome) and SARS (severe acute respiratory syndrome). The Sendai Framework makes far more mention of health than its predecessor the Hyogo Framework for Action, calling on countries to enhance the resilience of their health and medical systems, improve the DRR capabilities of personnel in the health and medical field, and provide communities with support.
The Framework urges countries to involve multiple sectors rather than just specific ones in reducing risks ("multi-sector approaches"). Once a disaster has occurred, be it natural or biological in nature, the impact reverberates across a variety of sectors such as infrastructure, water supply, education and health. Globalization, urbanization and modernization have led to more complex and compound disaster damage. Accordingly, plans that span a broad range of sectors are essential for preparedness, emergency responses, and recovery. The lessons learned each time a natural disaster strikes Japan or other countries have been used to reinforce the regimes set up for coordination and cooperation between sectors and organizations.
Risk reduction should be forthcoming not only from government institutions but from society as a whole. All organizations and individuals, including local governments, private-sector and civil society organizations, local communities, women and researchers, need to be involved at the national, regional and community levels and counted on to fulfill their respective roles and responsibilities. If a private company continues its business activities as far as possible during a disaster, for instance, it will be fulfilling its social responsibilities to safeguard employment and the local economy.
The approaches shown in this Framework have in fact been taken by countries as countermeasures against COVID-19. Entire societies are responding across numerous sectors with the aims of improving response capabilities and reducing harm. Applying the four priorities for action to coronavirus countermeasures, for example, would lead one to ask: (1) are the risks correctly understood and have warnings been suitably received, (2) have government programs and collaborative efforts with residents and other private-sector entities been put in place, (3) is there sufficient funding available, and (4) are response capabilities adequate?
Figure 1: The Sendai Framework's Seven Targets and Four Priorities for Action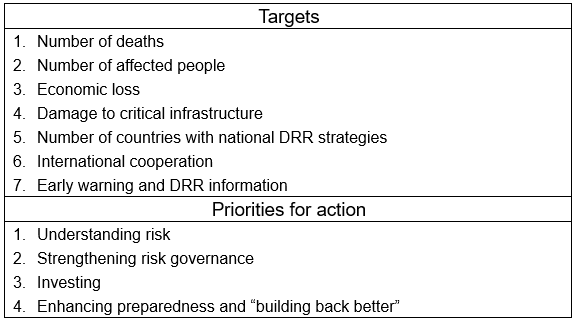
|
| Source: UNISDR (2015) as revised by the author2 |
Discussions on how best to pursue the Sendai Framework in the health field have led to the creation of a health framework. In 2016, the year after the Sendai Framework was adopted, the "Bangkok Principles for the Implementation of the Health Aspects of the Sendai Framework for Disaster Risk Reduction (2016)" were compiled primarily by experts in the health sector. Among the steps advocated were incorporating health/medical concerns into DRR policies/plans and DRR initiatives into health/medical policies, developing disaster-resilient health/medical systems, investing in health/medical infrastructure, strengthening capabilities, organizing and utilizing health data, and promoting science and technology. In 2019, the WHO put together the Health Emergency and Disaster Risk Management Framework that offered concepts and principles for managing public health risks stemming from infectious diseases, conflicts, natural disasters, industrial accidents and other hazards, and for effectively utilizing resources. The principles it presents include reducing risks in accordance with a society's vulnerabilities, enhancing preparedness rather than waiting to take action after a disaster strikes, preparing for all hazards, focusing on societies' vulnerabilities and capabilities, mobilizing the whole society and not just the health sector in responding to disasters, sharing responsibilities among all parties concerned (not only by the health sector), prioritizing risk management over post-disaster response, and seeking the participation of local communities.
2. The necessity of multi-hazard approaches to compound/cascading disasters
As socioeconomic structures have become increasingly complex, disaster damage has begun to impact more sectors and cause compound damage. The Great East Japan Earthquake of 2011 triggered a tsunami that set off a cascading reaction of nuclear accidents, large-scale fires, and fires at industrial complexes that in turn severed industrial production supply chains internationally, resulting in compound damage. Developing countries have at times not only been hard hit by flooding, earthquakes and other natural disasters, but also suffered the serious consequences of worsened hygienic conditions. More than 200,000 people were killed in the 2010 Haiti earthquake, and the subsequent cholera outbreak killed more than 9,000.
The COVID-19 pandemic has initiated a widespread cascading reaction that has prompted multi-hazard approaches. This has affected many other sectors and institutions outside the health/medical sector due to restrictions on employment, education, economic activities, finance and the movement of people. There are concerns that, if a large-scale natural disaster were to occur during a pandemic or if an infectious disease were to spread through refugee camps, responses would become all the more complicated and difficult. More than 800,000 Rohingya refugees that are housed in camps at Cox's Bazar in Bangladesh are being forced to prepare for cyclones in addition to COVID-19. Introducing social distancing rules at evacuation centers inside and outside Japan would greatly reduce housing capacity, and concerns about infections among disaster prevention personnel and volunteers have made securing personnel a challenge.
Multi-hazard approaches that cover increasingly complex disasters are deemed necessary. To develop systematic approaches, it is best to understand the frequency with which disasters occur and the envisioned damage, and then prepare scenarios. The risk when a compound/cascading disaster occurs can be expressed as follows:

|
|
Source: Hariri-Ardebili (2020) as revised by author3 |
Risk can be thought of as a ratio, with hazards that occur in compound/cascading fashion in the numerator, and the extent to which DRR capabilities have been built up as well as the extent to which these capabilities have been eroded by damage in the denominator. To reduce risk, DRR capabilities need to be improved, in other words, health/medical facilities and personnel need to be put in place and self-care and self-help capabilities enhanced. It is also essential to keep these capabilities from being undermined. These capabilities will be diminished, and risk will heighten, if health/medical or search and rescue personnel become infected by a virus, if medical/health facilities are damaged by flooding or earthquakes, if restrictions are imposed on the movement of relief supplies and personnel, or if a separate disaster occurs in the midst of a pandemic-caused shortage of medical resources.
Risks cannot all be reduced to zero, so one must be aware of trade-offs. Efforts are ongoing in Japan to minimize COVID-19 infection risks, including making evacuation at home rather than at an evacuation center an option when disaster strikes. When considering evacuation to escape flooding during a pandemic, the flooding may pose the greater risk (Table 1). A comparison of the risks indicates that the best response is to flee, to evacuate without hesitation. Recognizing the time differences in disaster timelines is also important. Responses to a natural disaster during a pandemic differ from the measures adopted to combat infectious diseases after a natural disaster.
Table 1: Risk comparison of COVID-19 and flooding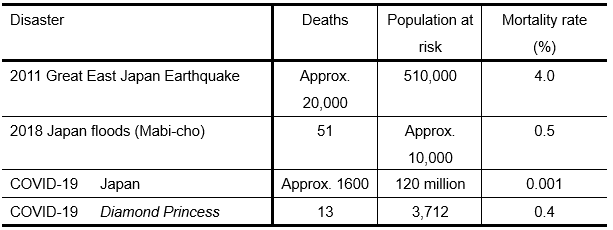
|
| Source: prepared by author |
3. Applying experience on reducing natural disaster risks to multi-hazard approaches
The insights and systems developed in reducing natural disaster risks can also prove useful for other disasters. Over its long history of fighting against natural disasters, Japan has reinforced its countermeasures every time it has suffered damage, and it now has in place a crisis management regime that might be termed a culture of disaster management. Asian countries, too, have put to good use the bitter experiences they have had with large-scale natural disasters such as the 2004 Indian Ocean tsunami and Cyclone Nargis (2008) to build up their laws, systems and organizations. These experiences and systems can be put to good effect in other disasters as well. Figure 2 shows a World Bank compilation of the lessons learned from the Great East Japan Earthquake, and it is clear that the COVID-19 pandemic shares these in common.
Figure 2: Lessons of the Great East Japan Earthquake Compiled by the World Bank
|
|
Source: Ranghieri and Ishiwatari (2014)4 |
While countermeasures naturally differ by disaster, they share many aspects in common. Table 2 compares the countermeasures to each type of major disaster, clearly showing that many of the activities are common, including the responses taken when disaster strikes, the stockpiling of supplies, and the restoration of livelihoods. In the wake of the massive fire that consumed the town of Itoigawa, Japan in 2016, relief efforts were carried out in accordance with the Disaster Relief Act. Despite the fact that it was man-made, the fire was treated as a natural disaster and the Natural Disaster Victims Relief Law was applied, which proved helpful in rebuilding housing. The job creation resulting from the emergency job creation/cash-for-work programs, the continued support for small and medium-sized enterprises provided through group subsidies, and the ICT-based matching of relief needs with supporters that were part of the recovery efforts following the Great East Japan Earthquake would likely also be effective as means of dealing with the COVID-19 pandemic. If evacuation centers are made available for use in natural disasters, then they can also be used as residential recuperation facilities for people afflicted with infectious diseases.
Table 2: Comparison of countermeasures by type of disaster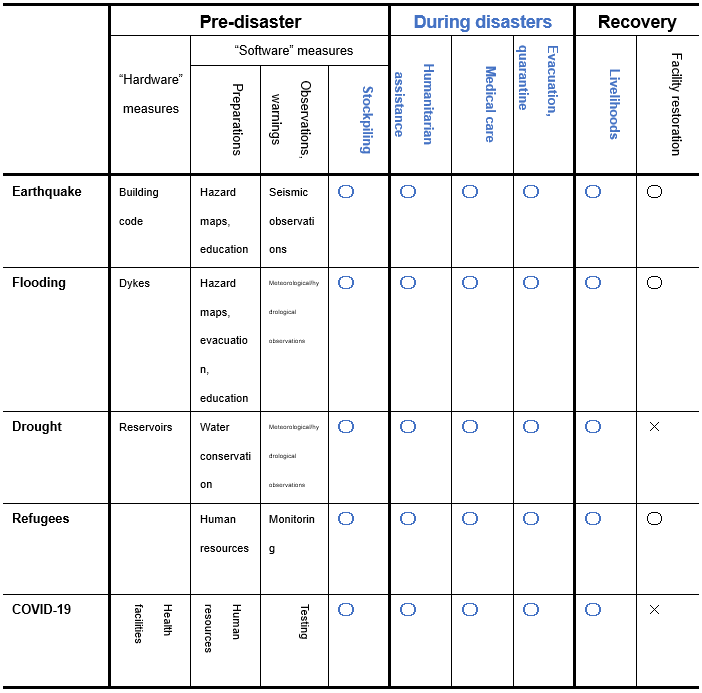
|
4. Steps being taken by DDR organizations to deal with the COVID-19 pandemic
Although the Sendai Framework highlights the importance of a multi-hazard approach, not many countries have in fact adopted this approach. Systematic approaches are needed; these might include ensuring the disaster management acts cover various disasters, having disaster management organizations coordinate all disaster countermeasures and including infection countermeasures into disaster management plans. Several countries have been managing disasters without distinguishing between natural disasters and biological disasters such as pandemics.
The Federal Emergency Management Agency (FEMA) performs comprehensive and centralized crisis management functions in the US. The 1988 Disaster Relief and Emergency Assistance Act covers biological disasters as well as natural disasters and accidents. The Pandemic and All-Hazards Preparedness Act was enacted in 2006, launching efforts to strengthen health security systems to deal with pandemics, bioterrorist attacks and all other disasters. Plans have been formulated, programs established, education/training undertaken, and crisis management regimes enhanced by (1) improving the functions and collaboration of relevant organizations, (2) utilizing ICT for remote medicine, etc., and (3) setting targets and allocating budgets. In responding to COVID-19, FEMA has procured medical supplies and deployed human resources, spending approximately US$5.8 billion (about 600 billion yen) as of May 2020 and utilizing disaster relief funds as well. Among the pending issues are concluding agreements for the procurement of supplies, clarifying the roles of relevant institutions, and assessing project effectiveness.
A disaster management law that also covers natural disasters was the basis on which a nationwide lockdown was imposed on India's population of over 1.3 billion. The National Disaster Management Authority is responsible for dealing not only with natural disasters but also with biological disasters. South Africa similarly declared a national state of emergency and ordered a lockdown that included a ban on the sale of alcoholic beverages and curfews based on its disaster management law. The prohibition on alcohol sales was aimed at reducing the harm associated with alcohol consumption and reducing the burden on hospitals. The Philippines is utilizing its National Disaster Risk Reduction and Management Council, whose chairperson - the Secretary of National Defense - is leading an inter-agency COVID-19 task force. DRR and management councils at the local government level chaired by governors and mayors are also being mobilized, especially in the distribution of relief supplies.
Japan is managing response to COVID-19 under a different structure than that used to deal with natural disasters. Developing infectious disease countermeasures is the responsibility of about 20 officials comprising the International Infectious Disease Control Coordination Office and the Office for Pandemic Influenza and New Infection Diseases Preparedness and Response set up by the Cabinet Secretariat in 2015 to deal with the Ebola hemorrhagic fever outbreak. A ministerial council was set up on January 21, 2020 and a panel of experts on February 14 to devise COVID-19 countermeasures. A new Office for Novel Coronavirus Disease Control was set up in March, and with a staff of about 70 at the end of July. On the other hand, natural disasters are the purview of around 100 personnel in the Cabinet Office who coordinate organizations concerned. The state of emergency that went into effect in April was declared on the basis not of the Disaster Countermeasure Basic Act that covers natural disasters but of the Special Measures Act to Counter New Types of Influenza.
5. Needed international cooperation
Multi-hazard approaches that include management of infectious diseases as called for by the Sendai Framework should be bolstered. As disasters have repercussions that set off cascading and complicating the damage, responses should be undertaken across numerous sectors spanning society as a whole. The experience garnered in dealing with natural disasters and the improved systems and mechanisms now available are not necessarily being put to full use by many countries in combatting COVID-19 infections. Greater international cooperation is needed.
An international multi-hazard knowledge center should be established. Countries have taken very diverse approaches in coping with COVID-19, with wildly varying degrees of success. It is essential that their countermeasures, structures and systems be analyzed and lessons drawn therefrom to enable them to improve their DRR approaches. International cooperation is needed to conduct research, offer advice and enhance capabilities regarding multi-hazards. Accordingly, an international center is called for that can bring together and consolidate knowledge and experience from those areas of endeavor in which individual countries are particularly proficient or successful so that these can be employed elsewhere. Japan has led the international community in developing more robust reduction to natural disaster risks, including by hosting the World Conferences on Disaster Risk Reduction. It should now take the initiative in promoting international cooperation to steadily implement the multi-hazard approaches recommended in the Sendai Framework.
1 The author would like to express his sincere thanks for the valuable advice extended to him in writing this paper by the members of the Global Issues Research Group, by Professor KANBARA Sakiko of the University of Kochi, and by NAKAMURA Shintaro, Senior Advisor, and KATSUBE Tsukasa, Senior Advisor, of the Japan International Cooperation Agency.
2 UNISDR (United Nations International Strategy for Disaster Reduction). 2015. Sendai framework for disaster risk reduction 2015 - 2030 . http://www.wcdrr.org/uploads/SendaiFrameworkforDisasterRiskReduction2015-2030.pdf .
3 Hariri-Ardebili, M. A. (2020). "Living in a multi-risk chaotic condition: pandemic, natural hazards and complex emergencies", International Journal of Environmental Research and Public Health, 17(16), 5635.
4 Ranghieri, F., & Ishiwatari, M. (2014). "Learning from megadisasters: lessons from the Great East Japan Earthquake", The World Bank.
![[Research Reports] Multi-hazard Approach to Compound/Cascading Disasters: Putting Experience in Developing Disaster Risk Reduction to Use in Pandemics](/eng/upload/eng/aflo_117014056eng.jpg)